You may have heard of endometriosis—but what about adenomyosis? Although the two conditions sound similar and can cause many of the same symptoms, adenomyosis is a separate and often misunderstood disease.
Wherever you are in your journey—whether you’re just beginning to understand your symptoms, searching for answers, or coming to terms with a diagnosis—we’re here to walk alongside you.
What Is Adenomyosis?
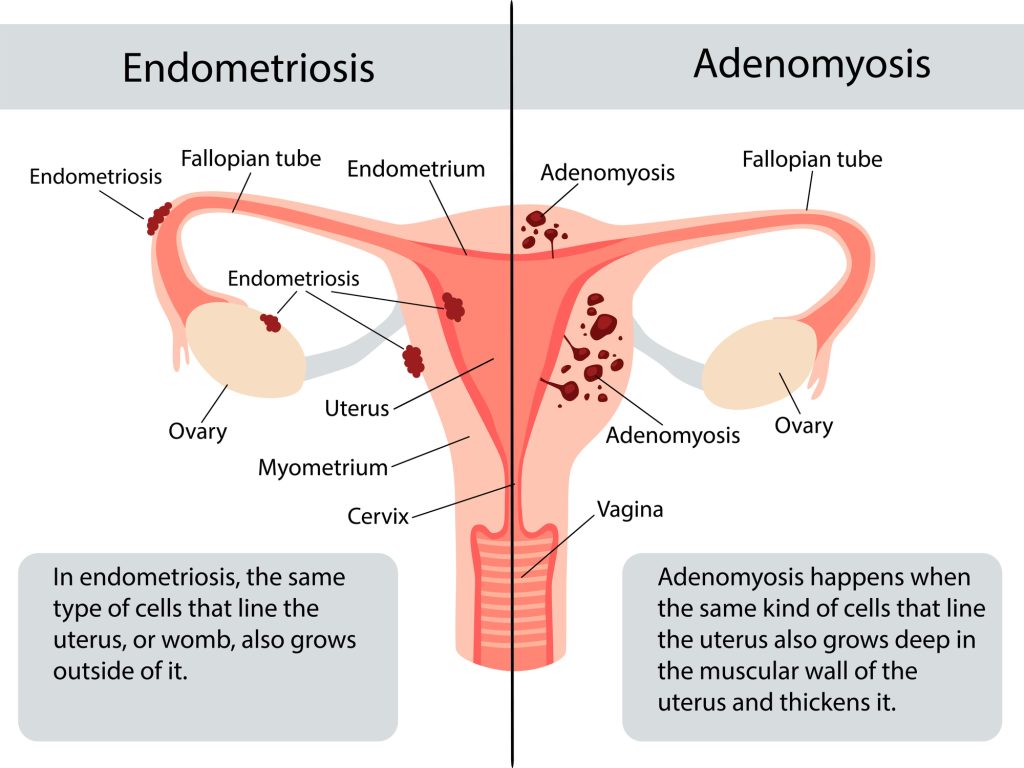
Adenomyosis occurs when endometrial glands or stromal cells grow into the muscular wall of the uterus, known as the myometrium. These cells behave similarly to regular endometrial tissue, which expands and contracts in response to fluctuating estrogen levels during the phases of the menstrual cycle. This thickening and bleeding of adenomyosis within the myometrium can cause severe uterine-centric pain.
Types of Adenomyosis
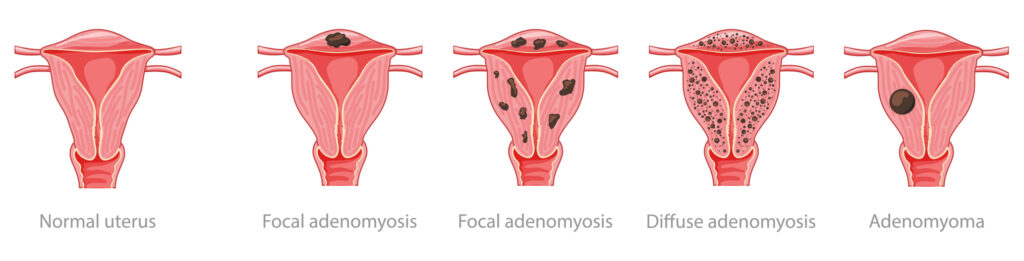
Adenomyosis can be diffuse or focal, depending on how the tissue spreads:
- In diffuse adenomyosis, the most common type, the endometrial tissue is spread out in many small spots throughout the uterine walls, often causing widespread pain and enlargement of the uterus.
- Focal adenomyosis is more concentrated—it looks like one or more small clumps or nodules of tissue instead of being spread everywhere. An adenomyoma is a specific type of focal adenomyosis where the misplaced endometrial tissue grows into a lump or nodule in one spot, and the surrounding muscle reacts by thickening even more.
You’ll also hear doctors and other experts talk about whether adenomyosis is in the inner or outer layers of the uterus. A special area in between these layers, called the junctional zone, is often thicker in people with adenomyosis, and that thickness is a clue for diagnosis.
Not sure which type of adenomyosis you have? Magnetic resonance imaging (MRI) scans can be a helpful next step for doctors to assess further.
Adenomyosis vs. Endometriosis
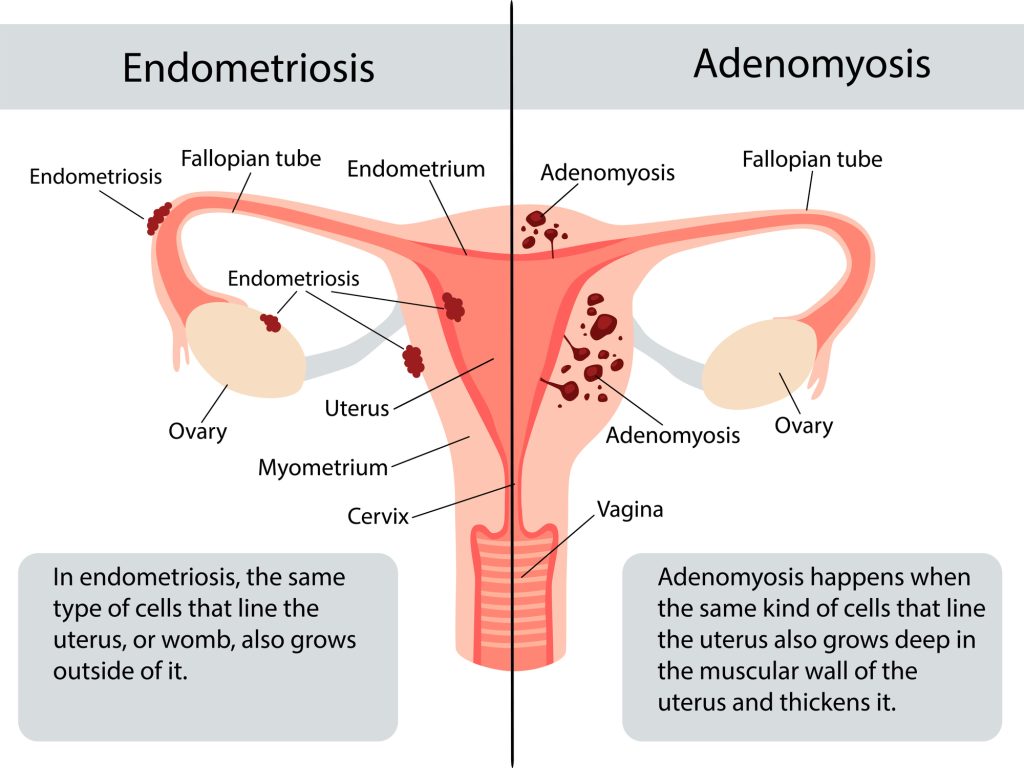
Understanding the difference between adenomyosis and endometriosis—and determining whether you have one or both conditions—can be confusing. Both involve endometrial-like tissue growing in places it shouldn’t. In adenomyosis, the tissue grows into the muscular walls of the uterus. In endometriosis, the tissue grows outside the uterus, on the surface of reproductive organs and on other organs throughout the body.
Adenomyosis is often described as the sister disease of endometriosis, as the two conditions frequently co-occur, although some patients may have one without the other.
Video: Can you have endo without adenomyosis or vice versa?
Adenomyosis vs. Uterine Fibroids
Unlike adenomyosis lesions, which consist of endometrial glands or stroma, uterine fibroids are benign (non-cancerous) masses or tumors that develop from normal uterine muscle. Fibroids are covered by a thin layer of connective tissue, known as the fibrous capsule.
Adenomyosis lesions, including adenomyomas, do not have this same fibrous capsule and most often occur throughout the uterine walls rather than in distinct masses or tumors.
Because both adenomyosis and fibroids affect the muscular walls of the uterus, both can cause abnormal thickening of the uterine walls.
Symptoms of Adenomyosis
Although some women with adenomyosis may experience no symptoms, adenomyosis often causes:
- Painful periods
- Painful intercourse
- Heavy menstrual bleeding with clotting
- Fullness, bloating, or a protruding abdomen, often called “adenomyosis belly”
- Chronic pelvic pain
Living with these symptoms can be physically painful and emotionally draining. Patients may miss school or work in the days leading up to their periods, when cramping tends to be strongest. Despite this, many patients tell us they felt dismissed or misunderstood before finding the right care. Remember: Your pain is real, and you deserve support.
Adenomyosis Causes and Risk Factors
While there are many theories as to why adenomyosis develops in some patients, its cause is not yet known. Researchers have identified several risk factors that correlate with a higher prevalence of the disease.
Adenomyosis is most commonly seen in women who:
- Are aged 40-50
- Have given birth (especially more than once)
- Have had previous uterine surgeries, such as Cesarean section or dilation and curettage (D&C)
- Have been diagnosed with endometriosis
Many women wonder if they can prevent adenomyosis. Because experts aren’t sure what causes adenomyosis, there is no known way to prevent the disease.
How Is Adenomyosis Diagnosed?
Though adenomyosis can only be confirmed with certainty after examining the uterus post-hysterectomy, experienced physicians can detect the signs of adenomyosis in several ways:
- Review of symptom and treatment history: Symptoms of adenomyosis can overlap with other conditions like endometriosis and uterine fibroids. Your doctor will want as much detail as possible about your symptoms and any diagnostic testing or treatments you’ve undergone thus far.
- Pelvic exam: A physical exam can help doctors determine whether your uterus is enlarged, which could indicate the presence of adenomyosis.
- Transvaginal ultrasound: A transvaginal ultrasound can show a bulky or asymmetrical uterus, cysts within the uterine muscle, or a thickened myometrium. Ultrasounds are affordable and accessible for many patients, but this lower-resolution imaging option doesn’t always provide the detail needed to diagnose adenomyosis.
- Magnetic resonance imaging (MRI): When ultrasound is inconclusive, an MRI can provide more detail. It’s especially useful for differentiating adenomyosis from fibroids and for mapping the extent of the condition, which helps guide treatment.
Reaching a diagnosis can feel like a long road, but it’s an important step toward reclaiming control of your health and finding relief.
Best Treatments for Adenomyosis
Deciding on treatment can feel overwhelming, especially when balancing immediate relief against future plans like pregnancy. While the definitive treatment for adenomyosis is hysterectomy (removal of the uterus), a knowledgeable care team can help you manage adenomyosis symptoms until you’re ready to explore surgery.
There’s no “right” choice—only what’s right for you at this moment in your life. You don’t have to treat adenomyosis if your symptoms are manageable, but if it’s interfering with your life, you don’t have to suffer through it alone.
Managing Adenomyosis Symptoms
If your symptoms are mild or moderate, medication is often the first step. Hormonal birth control (like the pill, patch, or hormonal IUD) may help lighten heavy periods and reduce pain by regulating or stopping your menstrual cycle. Gonadotropin-releasing hormone (GnRH) agonists, which put your body into a temporary menopause-like state, may be used for short-term relief in more severe cases. However, if you’re trying to get pregnant, birth control and GnRH agonists may not fit with your goals. Uterine artery embolization is a non-surgical procedure that blocks blood flow to the affected areas of the uterus, shrinking the tissue and reducing symptoms.
These treatments don’t “cure” adenomyosis, but they can help make life more manageable.
Surgery for Adenomyosis
Video: Is Surgery Possible for Adenomyosis If You Want to Get Pregnant?
In cases where symptoms are severe and other treatments haven’t helped, there are two surgical options:
- Adenomyomectomy is a surgical procedure that removes the areas of adenomyosis from the uterus while leaving the uterus itself intact. Unfortunately, adenomyosis frequently has irregular borders and tentacle-like infiltration into the uterine muscle walls, which makes it difficult to remove. For this reason, adenomyosis removal should be undertaken with extreme caution by an experienced surgeon, especially in a patient who desires pregnancy following the surgery. This surgery is typically only recommended in cases of focal adenomyosis if you plan to conceive afterward.
- Hysterectomy (surgical removal of the uterus) is the only treatment that fully cures adenomyosis. It’s usually recommended only when someone is finished having children and other treatments have failed to bring relief. Luckily, hysterectomy is a definitive cure for adenomyosis and can be performed using minimally invasive techniques that result in small incisions and minimal recovery time.
Dealing with adenomyosis can feel overwhelming, but you’re not alone. The best treatment plan is one that fits your lifestyle, your goals, and your body. A healthcare provider who understands adenomyosis can help you weigh the pros and cons of each option and find what works best for you—both now and in the future.
Adenomyosis Complications
Adenomyosis isn’t life-threatening, but if left untreated, it can seriously impact your quality of life. The condition doesn’t always get worse over time, but for many people, symptoms can become more intense and disruptive.
The most common complication of adenomyosis is iron-deficiency anemia due to chronic heavy periods. Anemia may leave you feeling tired, weak, short of breath, or dizzy. If not addressed, anemia can take a toll on your energy levels and overall health.
Can Adenomyosis Become Cancerous?
No, adenomyosis itself is not cancerous and does not turn into cancer. It doesn’t behave like cancer or increase your overall risk of developing uterine cancer in most cases. For the vast majority of people, adenomyosis is a chronic but manageable condition—not a precancerous one.
How Does Adenomyosis Affect Pregnancy?
Video: Can You Get Pregnant with Adenomyosis?
Adenomyosis doesn’t always cause fertility problems, but for some people, it can make it harder to get pregnant or carry a pregnancy to term. Some studies suggest that adenomyosis may be linked to pregnancy complications like miscarriage and preterm birth. However, many people with adenomyosis go on to have healthy pregnancies—especially with early diagnosis and supportive care. Your dreams of building a family still matter, and we’re here to help make them possible.
For those looking to get pregnant, hormonal therapy can help reduce inflammation and improve the uterine environment before trying to conceive. In some cases, adenomyomectomy can help. At ESSE Care, we recommend that patients wait at least six months to get pregnant after adenomyosis removal to allow the uterus to heal.
Get the Right Support for Adenomyosis
Adenomyosis can be frustrating and unpredictable, especially if you’re hoping to grow your family. But a diagnosis doesn’t mean you can’t get pregnant or live a normal life—it just means you may need a little extra support along the way. There are effective options to help you feel better, and the sooner you talk to a provider, the more control you can have over your care.
At ESSE Care, we see you as a whole person—not just a set of symptoms. We understand the physical and emotional toll adenomyosis can take, from missed opportunities to strained relationships. Our promise is not just medical expertise but genuine partnership on your path to healing.
Begin your ESSE Care journey today by reaching out for a personal case review.