Do you avoid intimacy because it’s painful? Does just the idea of intercourse make you anxious? Pain with intercourse (medically known as dyspareunia) is real, common, and significant—even though it’s often misunderstood.
What Does Painful Intercourse Feel Like?
Pain with sex can present in many different ways. Some common experiences include:
- Sharp or burning pain at the entrance to the vagina during initial penetration.
- Deep aching, pulling, or stabbing pain inside the pelvis, during or after penetration.
- Pain that radiates to the lower back, thighs, or pelvic floor muscles.
- Muscle spasms or a feeling of tightness in the pelvic floor during or after sexual activity.
- Pain occurring every time you try to have intercourse, or only in certain positions or at certain times.
- Emotional and relational effects, including fear of sex, anxiety about anticipation of pain, or avoidance of intimacy.
If you find yourself foregoing closeness, rearranging your life, or bracing for impact each time you consider sex, you’re not overreacting. This is a symptom worth exploring.
Why Does Painful Sex Happen?


At ESSE Care, we view dyspareunia not as an isolated issue but as a possible signal that multiple systems are involved. Many factors may contribute to pain with intercourse, and they often overlap:
- Entry pain (superficial dyspareunia): This may be caused by inadequate lubrication, skin or vulvar disorders, infections, hormone‑related vaginal dryness (especially during breastfeeding or perimenopause), or muscle guarding in the pelvic floor.
- Deep pain (deep dyspareunia): Often associated with conditions that affect the deeper pelvis, such as endometriosis, adenomyosis, fibroids, adhesions, pelvic floor dysfunction, or bladder or bowel‑related pain syndromes.
- Pelvic floor muscle dysfunction: Pain each cycle or from prior trauma may cause your pelvic floor to tighten or guard. Over time, this makes penetration or movement more difficult and painful.
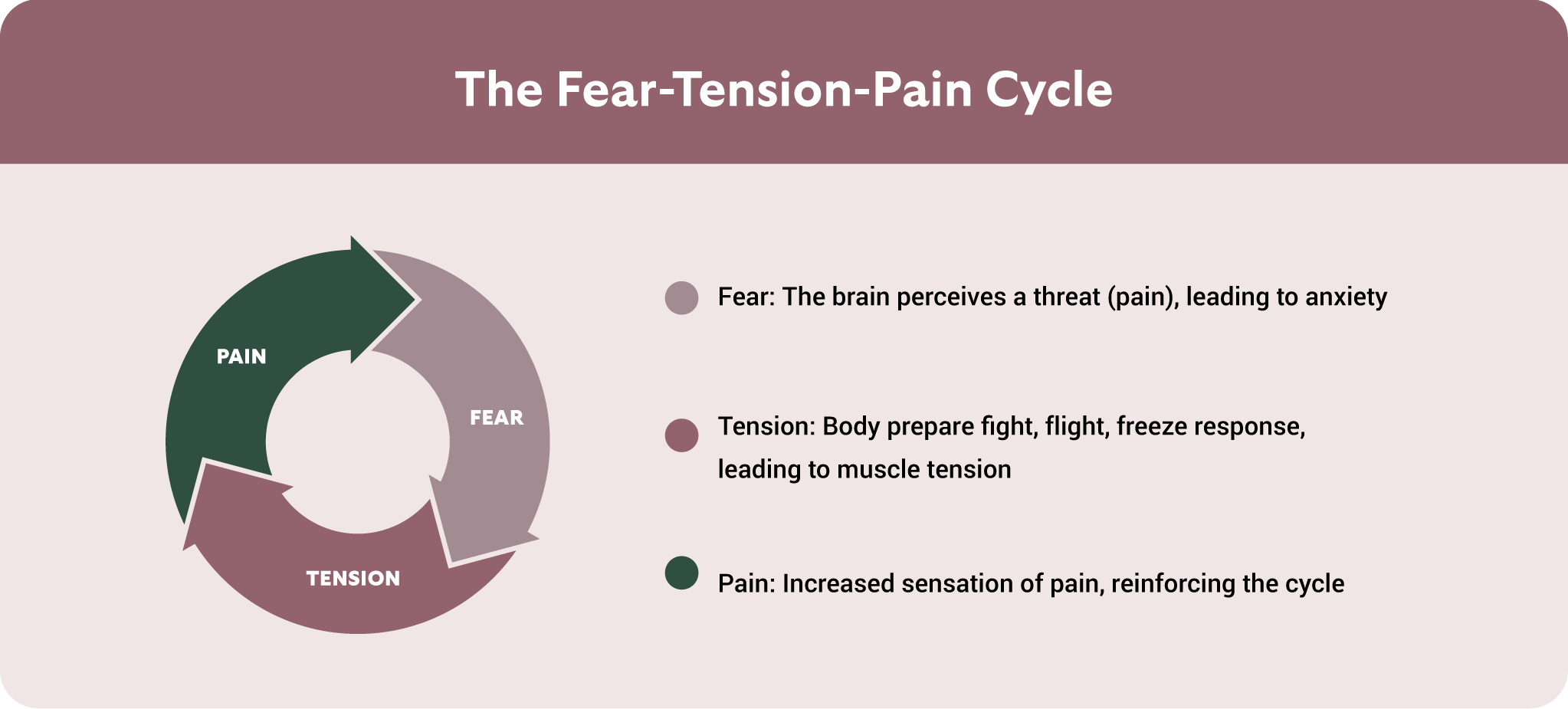
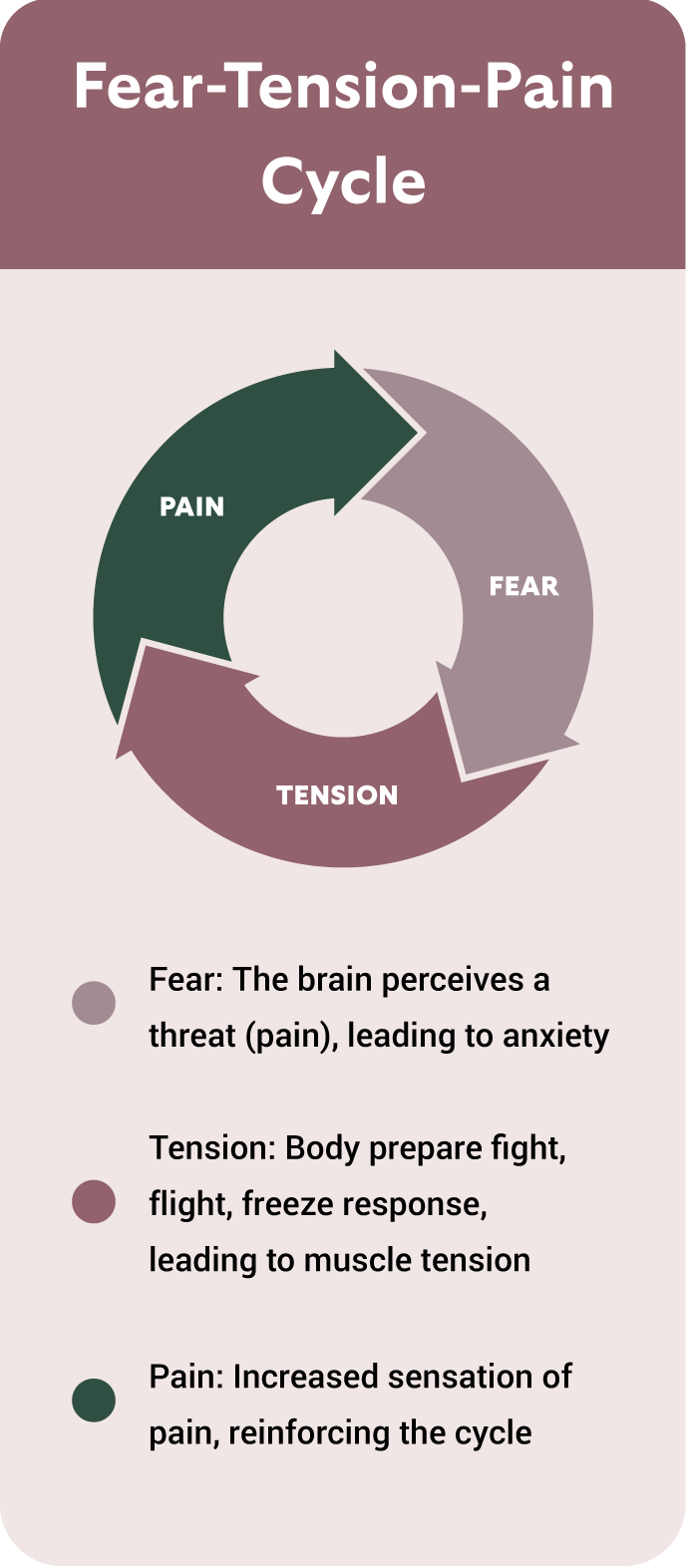
- Emotional, relational, or trauma‑related layers: Past sexual trauma, anxiety about pain, fear of penetration or performance, relationship stress—these all amplify the physical pain and make it harder to break the cycle.
- Other contributors: Vaginal anatomical variations, scarring from surgery or childbirth, genitourinary syndrome of menopause (especially in post‑menopausal or hormone‑suppressed patients), infections or skin conditions at the vulva, or neurological issues.
Because so many systems may be involved—muscles, nerves, hormones, organs—treating dyspareunia often requires an integrative lens.
When Should You Seek Specialist Care for Painful Sex?
If you’re struggling with pain or discomfort during sex, you deserve a full evaluation—not just reassurance or a prescription for lubricant. A specialist trained in advanced gynecologic care can help uncover the root causes of your pain and put together a treatment plan.
It’s time to see a specialist if any of the following is true for you:
- You have persistent pain during or after sex that impacts your life or relationship.
- You experience pain with tampon use, exams, or certain sexual positions.
- You’ve tried lubricants or hormones and still have discomfort.
- You have other symptoms, such as pelvic pain, bladder issues, painful periods, or known endometriosis.
- You feel tension, tightness, or involuntary muscle spasms in the pelvic floor.
- Your relationship is impacted by avoidance, fear, or emotional withdrawal due to pain.
You deserve an evaluation that listens to your experience. Pain with intercourse is not something you “just learn to live with.”
How We Approach Pain with Intercourse at ESSE Care
At ESSE Care, our approach to dyspareunia centers around your story, your body, and your goals. We will never dismiss your pain or suggest temporary solutions. Our aim, always, is to find the root cause and treat it. We bring together expert surgical, pelvic floor, integrative, and relational care to ensure we provide comprehensive, whole-body care.
The pathway often looks like this:
- Deep listening and detailed history: We always begin our new patient journey by obtaining a detailed symptom and medical history from our patients. We map out everywhere you feel pain, discomfort, or even just something “off” so that we can begin to piece together what systems of your body may be involved.
- Pelvic examination and muscle/fascial assessment: During a gentle pelvic exam, we look for signs of irritation or infection that could be causing superficial pain. We also assess the pelvic floor muscle tone, organ mobility, and areas of sensitivity to pinpoint any contributing factors to deeper pelvic pain. You are always in control—if an exam is causing you too much pain, you can always ask to stop.
- Targeted imaging and diagnostics (when needed): If there are signs of deep pain or suspected structural issues such as endometriosis, adenomyosis, or fibroids, we may order a transvaginal ultrasound or MRI and collaborate with other specialists, depending on the organs suspected to be involved.
- Pelvic floor physical therapy and integrative support: We partner with experienced pelvic floor physical therapists to release muscle spasms, retrain coordination, and support relaxation of the nervous system. Integrative support may include nutrition, mind-body work, trauma‑informed therapy, and sleep/stress optimization.
- Medical and surgical interventions when indicated: For some identified causes (e.g., endometriosis or adhesions), minimally invasive laparoscopy with excision may be recommended. For vulvar or vestibular (entry) pain, medical dermatologic or vulvar care may play a role. Lubrication, hormonal support, and local therapies are also part of the toolbox.
- Relational and sexual wellness support: Because painful sex affects more than the body, we also focus on communication, couples’ intimacy, exploring positions and practices that feel safe, gradual exposure, and rebuilding trust with your body and with sex.
- Long‑term follow‑up: Treatment is not a one‑time fix but a process of restoring function, comfort, connection, and confidence. We stay the course with you.
What You Can Do Right Now to Address Painful Intercourse
You don’t have to wait to be seen to take meaningful steps toward feeling better:
- Keep a sexual pain journal: Record when pain happens (entry vs. deep), what you do before/after, positions used, how you felt emotionally, and what seems to trigger or ease it. You can do this on paper or in a note on your phone/computer.
- Begin gentle pelvic floor awareness: Simple diaphragm breathing or supported stretches (hips and legs relaxed) can help loosen tension. See our partner article on pelvic floor care.
- Enhance comfort and safety: Use plenty of water‑based lubricant, focus on foreplay and arousal, try different positions that reduce pressure, and communicate with your partner about pacing and boundaries. (More tips on communication below.)
- Explore stress and relational context: Notice if you’re tensing up before sex, avoiding intimacy, or calming your body before penetration. Try a few minutes of mindfulness, meditation, or breathing together with your partner.
- Educate yourself: Learn more, ask questions, and advocate for yourself. Understanding yourself and knowing you’re not alone makes a big difference in how you feel. It can also help your care team understand you better and faster.
ESSE Care Tips: How to Talk to Your Partner About Painful Sex

Talking to your partner about sex can be uncomfortable even when nothing is wrong, so bringing up an issue like dyspareunia can feel overwhelming. But open communication will help your partner understand and support you as you find solutions together.
Here are five tips to prepare you:
- Take a deep breath. Remember that you deserve to enjoy sex as much as your partner does.
- Pick a time and place where you both feel calm and comfortable.
- Focus on “I” statements to avoid unintentional assignment of blame.
- Share any wisdom you’ve gained thus far about what is causing or contributing to your pain.
- Ask for what you need, whether that’s more lubrication, a slower pace, different positions, or activities that don’t involve penetration.
This will likely be an ongoing discussion, so don’t feel like you have to say everything at once. Often, the anticipatory anxiety is worse than the conversation itself.
You Deserve Connection Without Pain
Pain with intercourse impacts more than your body—it can affect your mental and emotional health, even outside the bedroom. You may have internalized the message that “everyone has pain” or “this just happens after surgery/children” or “I’ll get used to it.” At ESSE Care, we challenge that. You deserve sex that doesn’t hurt, and we believe relief is possible.
If you’re ready to explore what’s possible for you with a team that listens and cares deeply about your whole-body wellness, let’s walk that path together. Schedule a consultation with ESSE Care today.