If you’ve been avoiding sex because it hurts—or you’ve convinced yourself it’s just stress,” postpartum recovery, or something to push through—please know that painful sex is real, common, and treatable. Dyspareunia (pain with intercourse) affects physical, emotional, and relational well-being. Yet many people suffer silently, unsure who to turn to or what’s really causing the pain.
At ESSE Care, we believe deeply in the power of compassionate, specialized care. Pain with sex can stem from several overlapping causes—like endometriosis, pelvic floor muscle tension, hormonal changes, vulvar pain conditions, bladder or bowel contributors, and more—so quick fixes rarely solve the whole picture. Getting better starts with a team that listens, investigates root causes, and builds a plan around you.


Why Specialist Care Matters
It’s common to hear “everything looks normal” and leave with a lubricant or hormone cream. Those can help some people, but dyspareunia is often multifactorial, and deeper issues are easy to miss during brief, routine evaluations. A specialist trained in minimally invasive gynecology, pelvic pain, and integrative care is uniquely equipped to connect the dots across:
- Deep pelvic causes such as endometriosis or intrauterine adhesions (Asherman’s syndrome), often linked to deep penetration pain.
- Pelvic floor dysfunction overactive or tender muscles) that can make exams, tampons, or penetration painful.
- Hormonal contributors (postpartum, perimenopause, or menopause) where tissue changes raise the risk of dryness or burning.
- Coexisting bladder/bowel pain syndromes and central sensitization, which can amplify pain.
Pain with sex can show up in different ways. Specialist evaluation can prevent years of trial‑and‑error. For endometriosis in particular, addressing disease thoroughly via expert excision surgery can be pivotal when dyspareunia is part of the picture.
Who You Might See First and When to Go Further

Primary Care Providers
PCPs may rule out infections or prescribe basic treatments like lubricants or estrogen creams. While a helpful starting point, they aren’t set up to evaluate layered pelvic pain, so early referral is reasonable if symptoms persist or pain continues.
General OB/GYNs
They may perform pelvic exams, assess hormones, and order basic imaging which may identify conditions like uterine fibroids or ovarian cysts. However, routine evaluations often miss more complex conditions like endometriosis, Asherman’s syndrome, pelvic floor myofascial pain, or overlapping bowel/bladder issues.
Pelvic Floor Physical Therapists
These specialists can be critical in dyspareunia recovery. Pelvic floor physical therapy improves pain and function for many patients with dyspareunia. Still, PT alone may not be enough if deeper issues like endometriosis, adhesions, or nerve sensitivity are also present. That’s where coordinated specialist care matters.
Minimally Invasive Gynecologic Surgeons (MIGS)
This is where comprehensive care begins. MIGS specialists like those at ESSE Care combine surgical expertise, diagnostic acumen, and whole-person treatment to uncover and address the true drivers of pain. These experts can assess endo and other pelvic conditions, order targeted imaging, coordinate with pelvic floor physical therapists and other specialists, and perform advanced minimally invasive surgery when needed.
When to Seek a Specialist for Dyspareunia
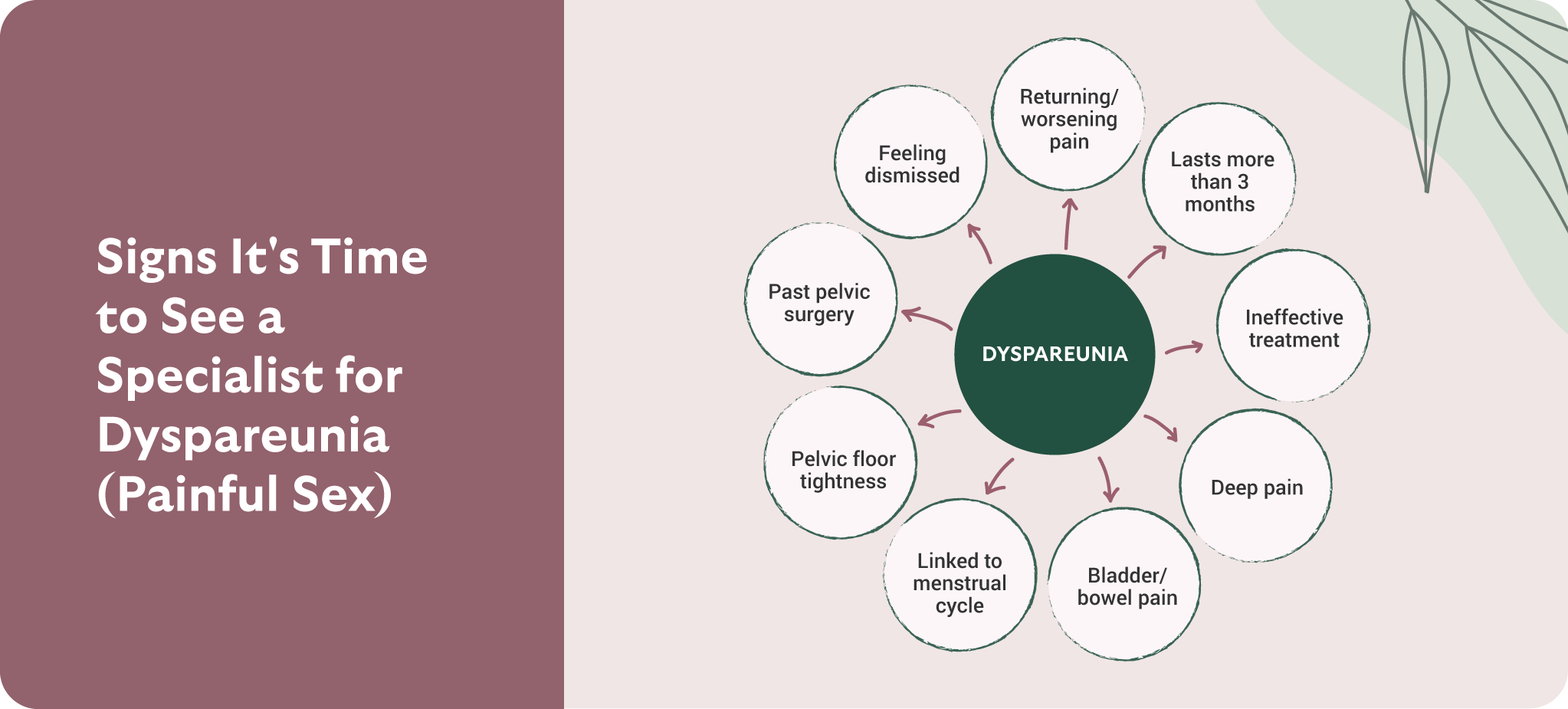
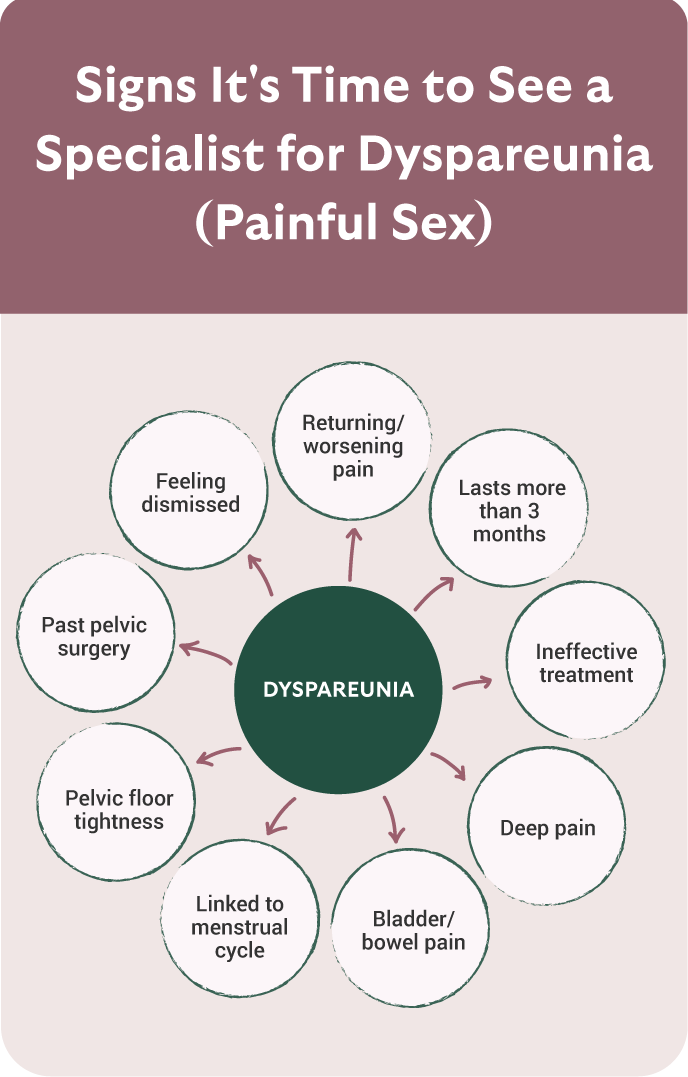
You don’t need to wait years—or for your relationship to suffer—to seek help. Consider specialist evaluation if any of the following apply:
- Pain during or after sex that keeps returning, is worsening, or lasts longer than 3 months.
- “Normal” exam but persistent pain, burning, or tightness—especially if lubricants or first-line measures haven’t helped.
- Deep pain with penetration, bowel symptoms, or cycle-linked flares that could indicate a pelvic condition like endometriosis.
- Pelvic floor symptoms, such as difficulty tolerating exams or tampons, muscle guarding, or tightness.
- Coexisting bladder or bowel pain, urinary urgency/frequency, or IBS-type symptoms.
- Past pelvic surgery or trauma, including pain after childbirth or history of endometriosis/fibroids.
- Feeling dismissed or stuck after multiple doctor visits—your experience is valid and deserves a thorough, trauma-informed approach.
What the Path to Specialized Care Can Look Like
| Step | What Happens | Why It's Important |
|---|---|---|
| 1. Recognition | You notice that sex is painful or triggering, or you begin avoiding it. | Pain is a signal, not a failure. You deserve to be heard. |
| 2. Initial Evaluation | PCP or OB/GYN rules out basic causes; you may try hormones or lubricants. | A useful start, but multifactorial pain often needs deeper evaluation. |
| 3. Referral to Specialist | You consult a MIGS/pelvic pain expert who takes a whole-body history. | Complex gynecology (including endometriosis) and pelvic floor issues require focused expertise. |
| 4. Comprehensive Exam | May include pelvic floor assessment, targeted imaging, and trauma-aware intake. | Identifies hidden causes and maps out a tailored plan. |
| 5. Multidisciplinary Plan | May include surgery, pelvic PT, hormones, or counseling. | Dyspareunia is multifactorial—your care should be, too. |
| 6. Follow-Up Support | Ongoing adjustments with a team that listens and measures what's improving. | Dyspareunia recovery is a journey—you shouldn't walk it alone. |
How to Advocate for Yourself
If you’re unsure how to begin this conversation, here are questions to bring to your next appointment:
- Could my pain be related to pelvic floor tension, endometriosis, or bladder/bowel pain?
- Do you offer specialized exams for pelvic pain (e.g., pelvic floor palpation) or can you refer me?
- What are the next steps if lubricants/hormones don’t work?
- Can I be referred to a pelvic floor physical therapist and a MIGS/pelvic pain specialist?
- How will this care plan align with my intimacy goals, fertility plans, and overall wellness?
If the answers don’t feel sufficient—or you feel dismissed—it’s time to seek a second opinion. You deserve better.
Our Approach to Dyspareunia at ESSE Care
We combine expertise and empathy to treat you, not just the pain.
Our whole-body approach and team include:
- Advanced gynecologic surgeons who are leaders in treating endometriosis and other pelvic pain causes like adhesions and fibroids.
- Pelvic floor physical therapists who specialize in trauma-informed, pain-aware rehabilitation.
- Counselors and coaches who help with the emotional and relational impacts of pain.
- Nutrition and integrative medicine partners who address inflammation and healing.
- A patient-centered, whole-body philosophy of care that puts the focus on your unique story and goals.
Ready to Reclaim Connection?
If painful intimacy has been weighing you down, you are not alone and you are not broken. With the right team and a tailored plan, relief is possible. We’re here to help you take the next step.
Schedule a consultation with the ESSE Care team today and begin your path to healing.



