If sex has become something you brace for instead of something you enjoy, or if intimacy feels more like a trigger than a connection, you’re not alone, and you’re not overreacting.
Dyspareunia, the medical term for painful sex, is far more common than many realize, affecting nearly 3 in 4 women over the course of their lives. Yet it’s often misunderstood or dismissed. At ESSE Care, we take dyspareunia seriously—because it affects not just the body but also personal relationships and emotional well-being.
Symptoms and Types of Dyspareunia
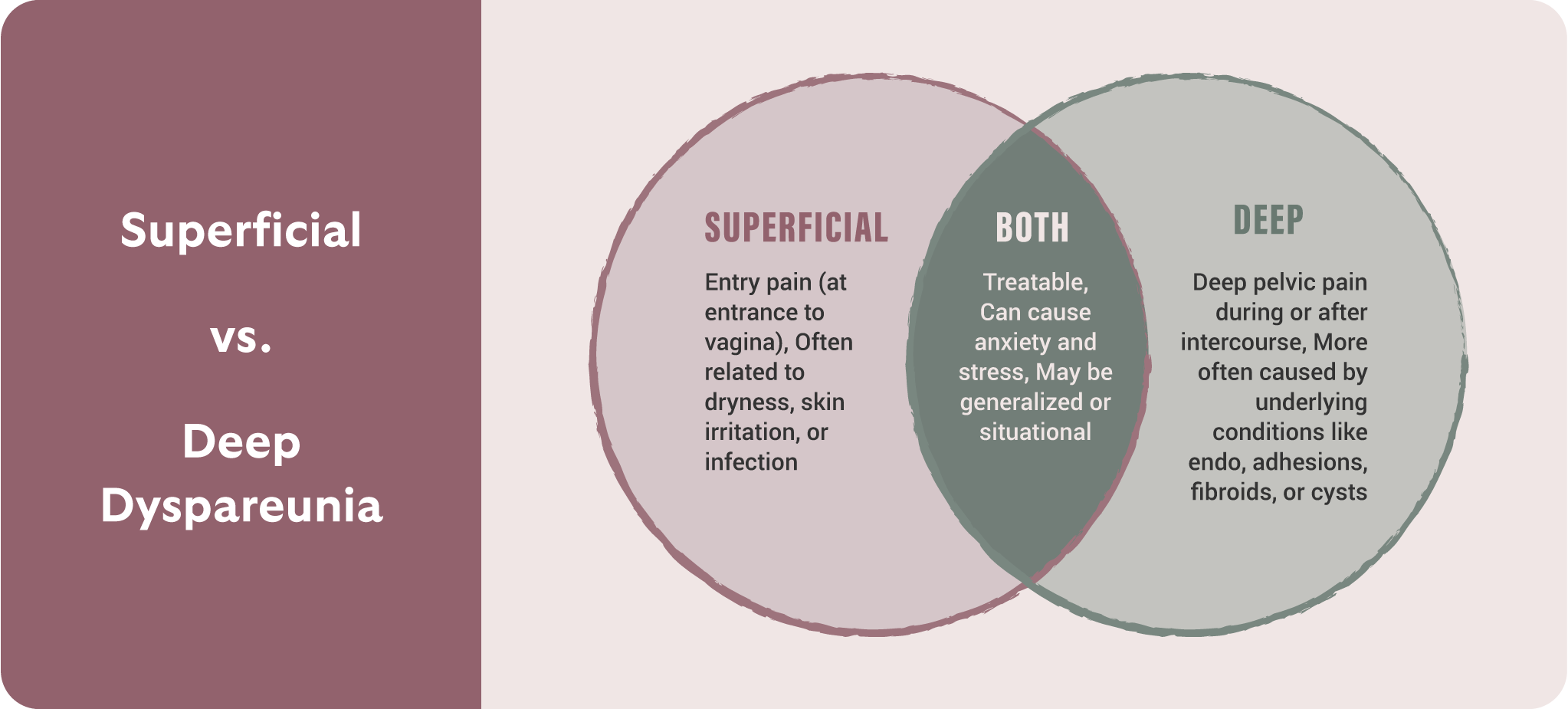
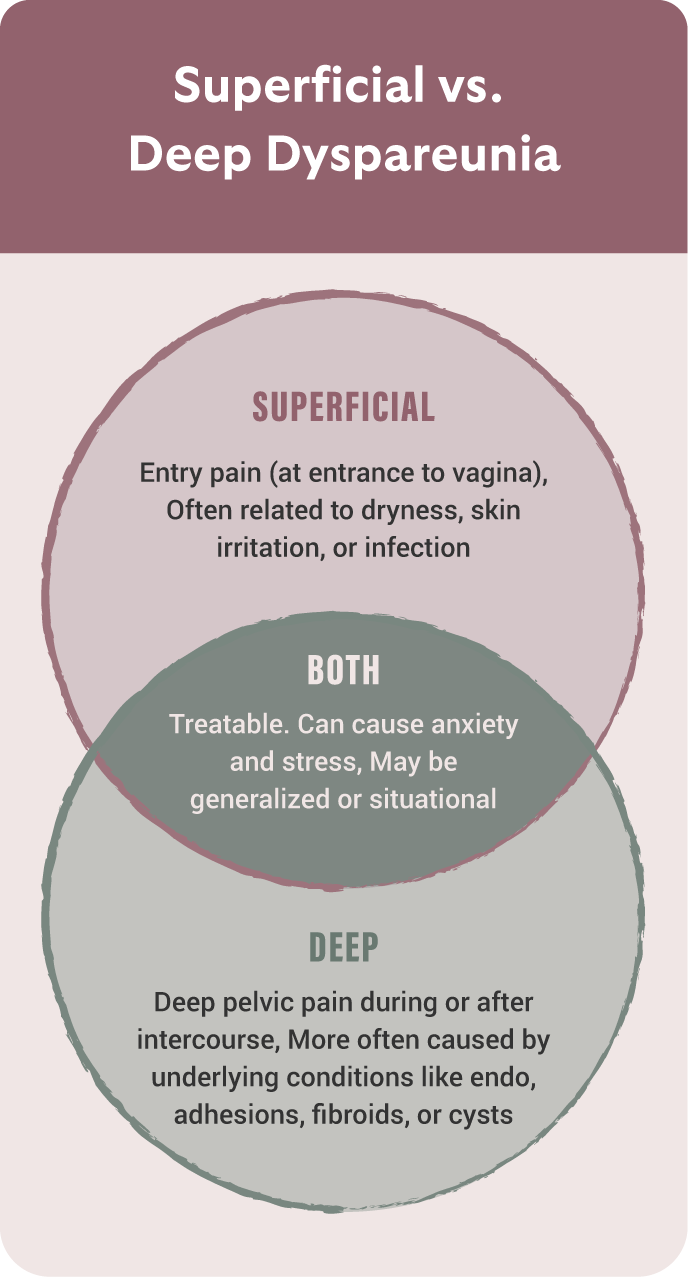
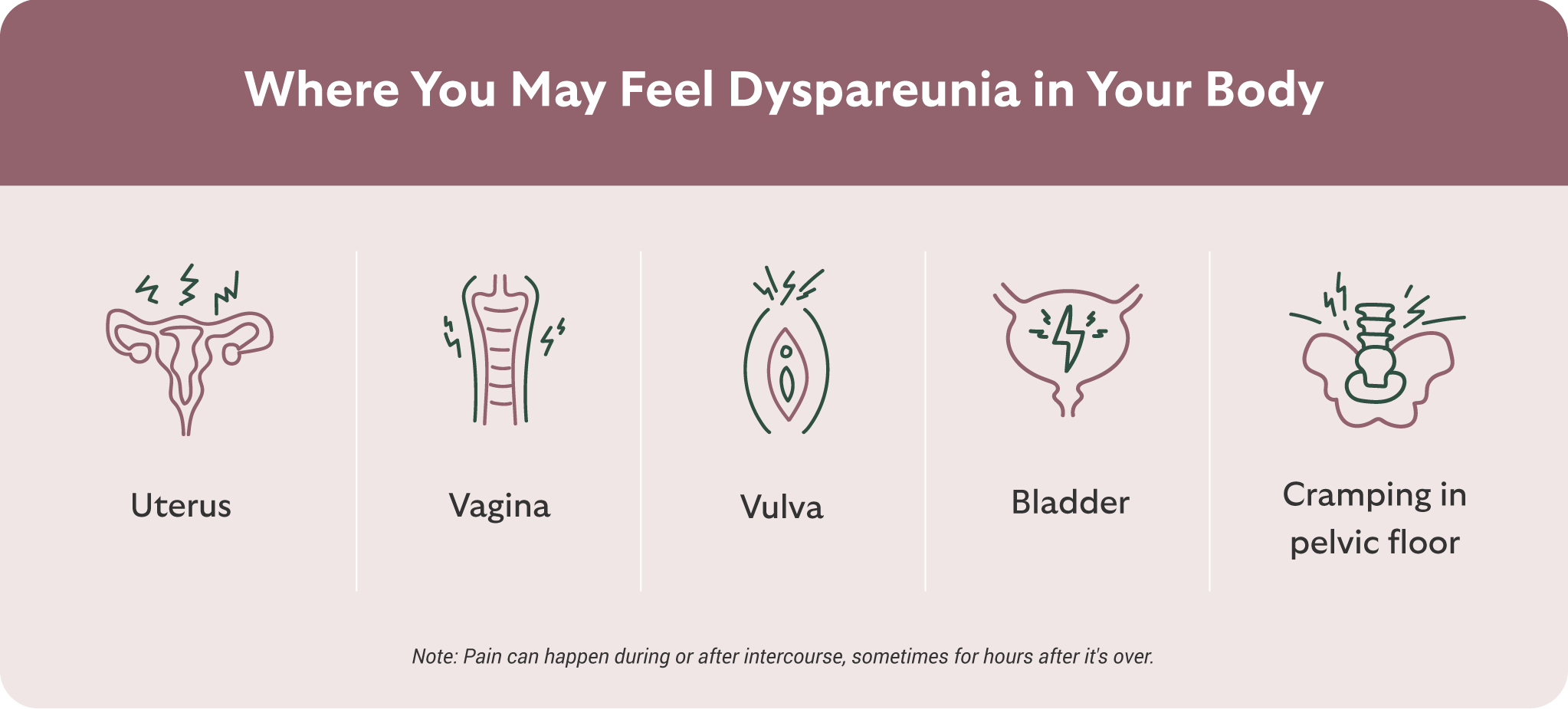
There’s no universal version of dyspareunia. For some, pain occurs only with initial penetration; for others, it’s deep pelvic pain during or after sex. Still others feel aching, burning, or cramping that lingers long after intimacy has ended. It can also radiate to other areas of the body, such as the lower back, hips, or thighs.
People with dyspareunia may also experience pain with tampon use or during pelvic exams.
Here’s a breakdown of the different types of dyspareunia, which can help you have the right vocabulary when talking to your provider:
- Superficial: Sharp or burning pain at the entrance to the vagina, often upon initial penetration.
- Deep: Aching or pulling pain inside the pelvis during or after sex.
- Primary: Pain felt since first sexual experience.
- Secondary: Pain that emerged after previous pain-free experiences.
- Generalized: Pain that always happens, no matter the partner, type of sexual contact, or environment.
- Situational: Pain that only occurs with certain people or situations.
If you find yourself avoiding sex, adjusting your relationship, or dreading intimacy because of pain, that is not “normal.” It’s a signal that your body deserves attention.
Causes of Dyspareunia


At ESSE Care, we view dyspareunia as a multifactorial condition. This means multiple body systems—including muscles, nerves, hormones, anatomy, and emotions—often play a role. That’s why we never offer a one-size-fits-all answer.
Some of the potential causes of painful intercourse include:
- Gynecologic conditions: Endometriosis, adenomyosis, uterine fibroids, adhesions, ovarian cysts, and other conditions can cause acute or chronic pain in the pelvic and vaginal areas.
- Infections: Yeast infections, pelvic inflammatory disease, and skin infections can all cause pain in the vagina and vulva.
- Sexual response dysfunction: Lack of desirer arousal caused by a mix of physical and psychological factors.
- Hormonal changes: Particularly Genitourinary Syndrome of Menopause (GSM), where decreased estrogen levels lead to vaginal dryness, irritation, and painful intercourse.
- Childbirth: If you had an episiotomy or tear during childbirth, you may experience pain for several months afterward while you heal.
- Anxiety: Once you’ve experienced painful sex, your pelvic floor may tense up involuntarily (known as vaginismus), or you may have trouble with sexual response due to fear of additional pain. (Note: This does NOT mean the pain is “all in your head”!)
- History of trauma or abuse: Similar to anxiety, past sexual trauma can lead to tightness and pain during sex.
- Emotional and relational factors: Stress and conflict in the relationship is an underestimated cause of pain and discomfort.
- Other physical factors: Inadequate stimulation or lubrication before penetration.
- Unknown causes: Chronic pain conditions like vulvodynia sometimes don’t have a known cause, but that doesn’t mean the pain isn’t real.
Remember, there are often multiple factors contributing to pain during sex, so it’s likely that your discomfort is related to more than one of the causes above.
How Is Dyspareunia Diagnosed?
Diagnosis is—or should be—simple: If you experience pain during sex, you have dyspareunia.
But seeking a specialist to identify the underlying cause of your pain requires additional measures. These might include:
- Seeing a gynecologist and providing a detailed history of your pain and other symptoms.
- Pelvic floor assessment and/or a gentle pelvic exam (if you are able).
- Pelvic ultrasound or MRI to evaluate for endometriosis, adenomyosis, or fibroids.
- Referral to dermatology or vulvar specialists for skin-related pain.
- Neurologic assessment in cases of persistent nerve-based pain.
Treatment Options for Painful Sex
The appropriate treatment for dyspareunia will depend on your diagnosis, but options may include:
- Hormonal support: Topical or systemic therapy for GSM or dryness.
- Surgical care: For underlying pathology such as endometriosis or adhesions.
- Pain management strategies: Including neuropathic medications when appropriate.
- Pelvic floor physical therapy: Relaxation techniques, nervous system regulation, and pain processing to address muscle tension, spasms, and pain patterns.
- Counseling or therapy: To process trauma or relational strain and receive guidance on communication with your partner about painful sex.
How ESSE Care Approaches Dyspareunia
Our approach is rooted in listening. We begin by asking questions to understand:
- How and when the pain started
- Whether it’s superficial, deep, or both
- Your hormonal context (e.g., postpartum, perimenopause)
- Prior trauma, childbirth, or pelvic surgery
- Emotional and relational impacts
We use all the diagnostic tools at our disposal—physical exam, imaging, symptom mapping, and specialist referrals—to identify what is causing your pain and what might resolve it.
It’s important to remember that dyspareunia is rarely resolved in a single visit. We create a whole-person care plan that includes ongoing pelvic rehab and adjustments to treatment as your needs evolve.
Stop Suffering Through Intimacy
Sexual pain can be isolating. It affects how you see yourself, how you relate to others, and how you feel in your own skin. But healing is possible with the right care and a supportive team that honors your story.
At ESSE Care, we believe in a new narrative: One where intimacy feels safe, your body feels like home, and you have agency in your healing.
If you’re ready to explore what’s next, we’re here, and we’re ready to help. Take the first step by scheduling a consultation.