Endometriosis is often discussed in terms of pain. But as explored in Episode 8 of The Endo Exchange, its impact extends far beyond physical symptoms.
This multidisciplinary webinar, hosted by Dr. Karli Provost Goldstein of ESSE Care, featured a conversation with Dr. Mary Sabo, an expert in acupuncture and Chinese medicine, and Batya Novick, a therapist specializing in reproductive mental health. The session brought together perspectives from surgical care, integrative medicine, and reproductive mental health to explore how endometriosis affects daily life, relationships, fertility, and emotional well-being.
This article highlights the most important insights from that discussion, grounded in both clinical expertise and patients’ lived experiences.
1. Endometriosis often begins early, but the signs are frequently dismissed.


For many patients, symptoms begin in adolescence with painful periods (dysmenorrhea). Severe or disruptive period pain is not considered normal, yet it is frequently minimized by family members, peers, and even healthcare providers. This early dismissal can lead to years of delayed recognition. In fact, teens often wait up to 5.4 years for a proper diagnosis of their pelvic pain, compared to 1.9 years for adults.
What this can look like:
- Missing school, sports, or social events due to pain
- Vomiting, fainting, or being unable to function during a period
- Frustration or confusion from being told symptoms are “just part of being a woman”
Dysmenorrhea is not just a physical burden; it can deeply affect emotional wellbeing, relationships, education, and career aspirations. Among adolescents, it is the leading cause of short-term school absenteeism. Many young people lose multiple days each month to pain, yet nearly 25% never discuss their symptoms with a healthcare provider.
Frequently missing school and social events can affect confidence, academic performance, and social development. These are years young people can never get back.
2. Chronic pain changes how the body responds over time.


When pain repeats month after month, the body begins to adapt in ways that go beyond the reproductive system.
The webinar discussion highlighted how endometriosis affects the nervous system, sleep, digestion, and overall pain processing.
This can show up as:
- Persistent fatigue and disrupted sleep patterns
- Digestive symptoms and food sensitivities
- Increased sensitivity to pain
- A constant “fight or flight” stress response
Over time, the body may begin anticipating pain, which can amplify symptoms even outside of the menstrual cycle.
This is why care should address both physical disease and nervous system regulation.
3. The emotional and psychological impacts are often overlooked.
Endometriosis can shape how someone relates to themselves, and not for the better.
Many patients spend years navigating symptoms without answers, which can lead to:
- Anxiety and chronic stress
- Feelings of isolation or not being believed
- Loss of trust in their body
- Challenges with intimacy and relationships
This pattern is especially common in patients with long histories of symptoms that were never diagnosed. But even for those who only discover endometriosis during fertility struggles, realizing they’ve been dealing with a silent disease for years can be destabilizing. In both cases, the emotional impact can be significant and long-lasting.
Mental health support is an essential part of care, not a separate piece.
4. Many patients only get answers after years of misdiagnosis.
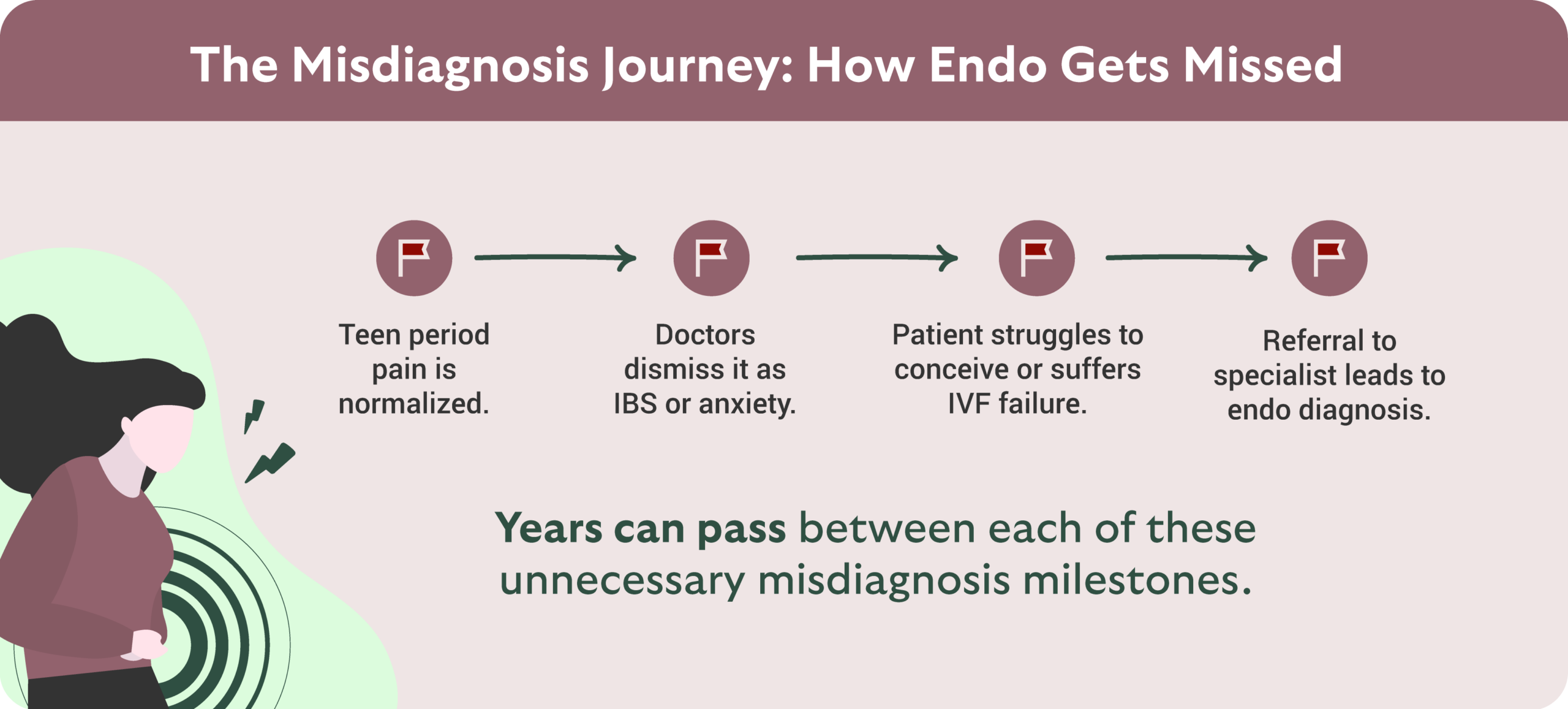

A major theme throughout the conversation was how long it often takes for endometriosis to be recognized. Patients are frequently given many other erroneous explanations before endometriosis is even considered.
Common misdiagnoses may include:
- Gastrointestinal conditions like IBS
- Anxiety or stress-related diagnoses
While some patients continue to advocate for themselves, others may accept a provider’s misdiagnosis (and continue to suffer) because they assume the provider knows best. Unfortunately, those without advanced endometriosis training often miss subtle signs of the disease, believing that normal-looking scans mean no disease is present. (Spoiler: This couldn’t be further from the truth.)
If you or your child is on a journey to find answers, remember that laparoscopy is the only definitive way to diagnosis (or rule out) endometriosis.
5. Real progress happens through multidisciplinary care.
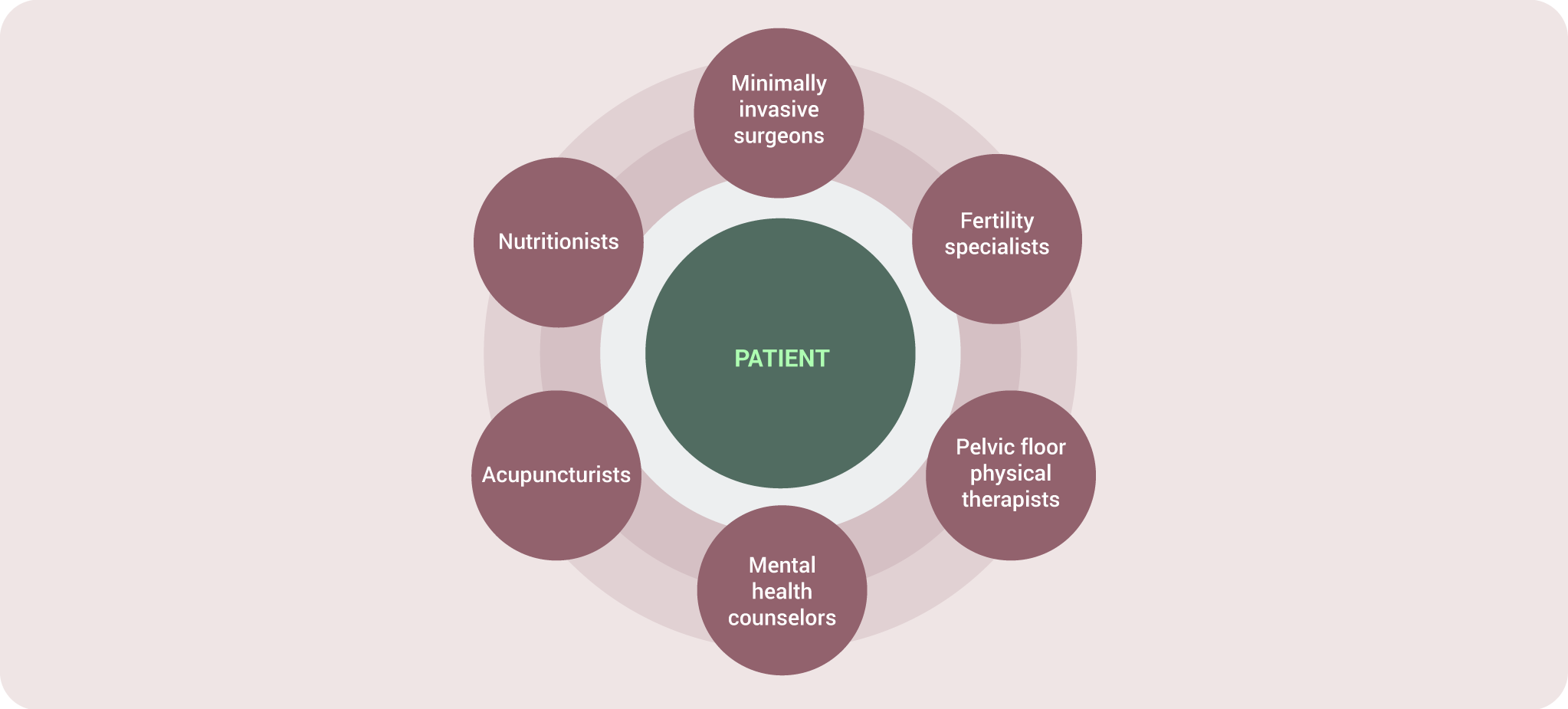
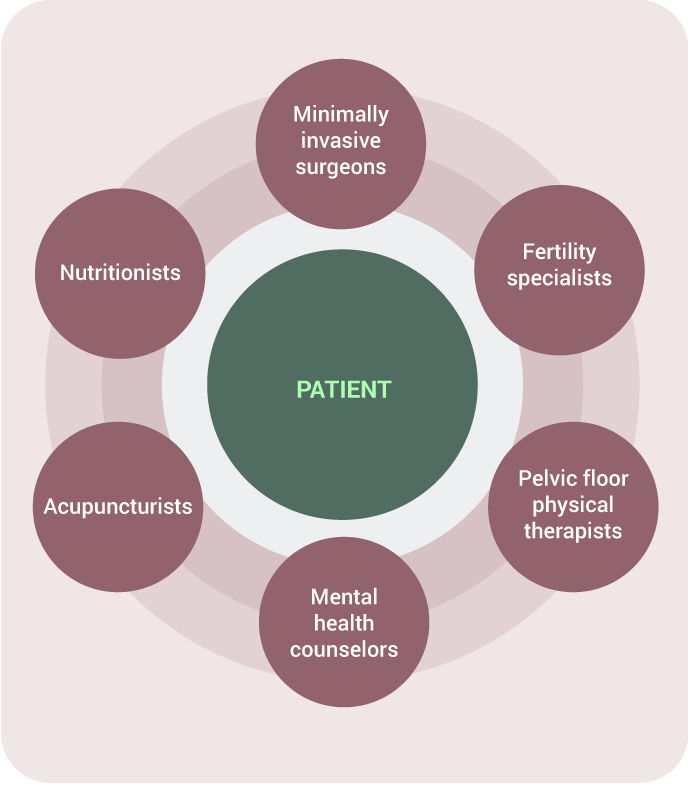
One of the most consistent messages from the panel was that endometriosis care cannot exist in silos. Effective care involves collaboration across specialties to support the full patient experience.
This may include surgical care for diagnosis and excision, fertility specialists when needed, integrative therapies to support the nervous system, pelvic floor physical therapy, and mental health support.
This approach helps address physical symptoms and inflammation, nervous system regulation, emotional well-being, and long-term quality of life. Patients benefit most when care is coordinated and centered around the whole person.
What This Means for Your Care
Endometriosis is not just a condition. It is an experience that can affect every part of life.
If you are navigating symptoms, these reminders may help guide your next steps:
- Pain that disrupts your life is not normal.
- You deserve to be heard, even if tests are inconclusive.
- Symptoms may involve more than one system in the body.
- Mental health support is a key part of care.
- Seeking additional opinions is valid and often helpful.
At ESSE Care, conversations like this one continue to shape how we approach endometriosis care. The discussion in Episode 8 of The Endo Exchange reflects a commitment to understanding the full impact of this disease and supporting patients with thoughtful, collaborative care.
Healing is not just about treating the disease. It is about restoring quality of life, rebuilding trust in your body, and creating a path forward with the right support.



