What Arleigh’s Story Reveals About Whole-Body Healing
In our Whole-Body Care & Wellness for Endometriosis webinar, we brought together an interdisciplinary panel to explore how integrated care transforms outcomes. Alongside expert voices in surgery, pelvic floor therapy, and nutrition, we were honored to welcome someone whose experience reframed the entire conversation—Arleigh Cole, Certified Health Coach and Patient Advocate.
Arleigh joined the webinar not as a clinician, but as a patient. Her story grounded everything we discussed in one core truth: real healing starts with being believed.
A Common Story, Told Too Often
Arleigh’s endometriosis journey began long before she had a name for it. She lived for years with symptoms that disrupted her life but didn’t show up on standard labs or imaging.
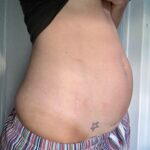
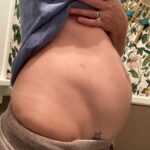
- Daily bloating and sharp pelvic pain, especially mid-cycle and during menstruation
- Digestive issues that were brushed off as IBS—constipation, post-meal cramping, and challenges of severe constipation
- Painful sex, something she was told was “normal” for some women
- Chronic fatigue that wasn’t improved by sleep, diet changes, or medications
- Anxiety and overstimulation that often flared around hormonal shifts
She saw GI doctors. She was referred to OB/GYNs. She was told to try birth control. She was prescribed antidepressants. She was assured everything was “normal.”
This happened because her care was fragmented—each system treated in isolation, while the full picture of endometriosis remained unseen.
The Turning Point: Whole-Body Listening
It wasn’t until Arleigh found her way to Dr. Karli Provost Goldstein and the ESSE Care team that she experienced a different kind of care—care that connected the dots.
Through consultation, detailed history-taking, and advanced imaging, Arleigh’s symptoms were reevaluated through the lens of endometriosis. Her GI pain wasn’t just IBS. Her pelvic pain wasn’t just “bad periods.” Her nervous system hypervigilance wasn’t just anxiety.
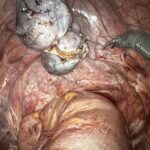
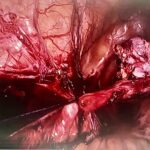
She underwent laparoscopic excision surgery, which revealed deep infiltrating endometriosis involving her bowel, pelvic sidewalls, and pelvic nerves—lesions that had likely been contributing to years of pain, fatigue, and dysfunction.
But the treatment didn’t stop at surgery.
Some of her care plan included:
- Pelvic floor physical therapy, to help release the guarding and hypertonicity caused by years of unmanaged pain and nervous system overload
- Functional nutrition, focused on reducing systemic inflammation, supporting hormone detoxification, and healing her gut after years of antibiotic use and restrictive diets
- Post-op integrative support, including movement, breathwork, and nervous system regulation to reduce flare-ups and support healing from medical trauma
This worked because her symptoms were seen as part of a whole-body picture—and treated in coordination, not isolation.
Empowering Others Through Advocacy
Today, Arleigh works with patients who are still where she once was—searching for clarity in a system that often downplays or fragments their experience. As a Certified Health Coach, she helps patients navigate their appointments, understand their treatment options, and rebuild their confidence after years of being dismissed.
In the webinar, she offered specific, real-world guidance for those just beginning their journey—or struggling to feel seen in their care.
What Arleigh Wants You to Know
Arleigh’s insights weren’t abstract—they came directly from what she wished someone had told her earlier in her process.
1) Trust what your body is telling you.
Even when tests come back normal. Even when a provider tells you it’s “nothing.” If your symptoms are interfering with your life, they’re real. Don’t wait for outside validation to keep asking questions.
2) Track everything.
Arleigh began tracking her bloating, bowel movements, fatigue, and pelvic pain alongside her cycle. This pattern recognition gave her powerful language in appointments—and helped her providers understand what was being missed.
3) Prepare and slow things down.
She encourages patients to bring symptom logs, write down questions, and ask providers to pause and explain recommendations. You can say:
- “I need time to process that.”
- “Can you explain the reasoning behind this treatment?”
- “What are the alternatives?”
4) You don’t have to stay where you’re not heard.
Arleigh described the emotional weight of staying too long with well-meaning providers who simply didn’t understand endo. The relief of finding a care team that did was profound—and it only happened when she stopped settling for care that wasn’t working.
5) Community makes the process sustainable.
Whether through endo support groups, peer advocates, or a practice like ESSE that truly integrates whole-body care, she encourages patients to surround themselves with people who listen without minimizing. Healing takes support.
Why Her Story Belongs in the Conversation
Arleigh’s voice in the webinar reminded us that no treatment plan is complete without the patient’s perspective. She helped bridge the clinical conversation with the emotional, daily realities of what it feels like to live with invisible pain.
She also reinforced that healing isn’t just physical—it’s relational. When care is built around collaboration, trust, and validation, it doesn’t just treat the disease. It restores the person behind it.

Building a Future Where Advocacy Is Standard
At ESSE Care, we don’t see advocacy as separate from medicine—it’s part of it.
Arleigh’s story showed what’s possible when the right team listens to the full story:
- Her bowel symptoms were finally connected to deep endo involvement
- Her nervous system flares were treated as part of the picture, not dismissed as anxiety
- Her fatigue and GI distress were acknowledged as real, complex, and worthy of comprehensive care
- And most importantly—her voice was central to the entire process
We’re proud to work with Arleigh not just as a former patient, but as a partner who supports others navigating the same road she’s walked.
At ESSE, we believe your experience belongs in the room. Your story informs your care. And your advocacy is not a bonus—it’s a vital part of your healing.
If you see yourself in Arleigh’s story, you’re not alone.
We invite you to connect with us. Explore our integrated, patient-centered approach to endometriosis and pelvic pain—and let us meet you where you are, with care that listens, responds, and empowers.



